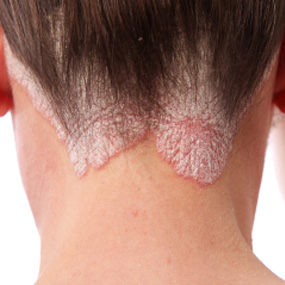
Psoriasis is a skin condition that affects approximately 7.5 million people in the United States, according to the American Academy of Dermatology. The telltale symptoms are patches of skin that look pink or red and scaly with a silver coloring on top. The most common type is called plaque psoriasis and usually occurs on body parts like the knees, elbows, and/or scalp.
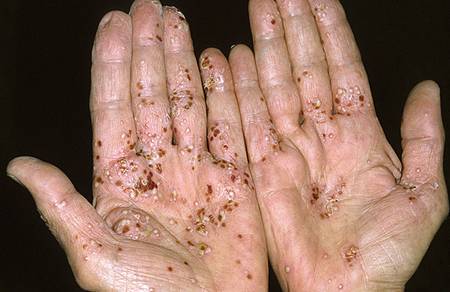
Scalp psoriasis, in particular, has some unique treatments that include shampoos and solutions. If you have plaque psoriasis on other areas of the body, beyond the scalp, here’s how a dermatologist (a doctor who specializes in the skin) would generally approach treatment.
Psoriasis treatment overview
A dermatologist considers several factors during a physical exam before figuring out a treatment regimen. “It can depend on the severity of the psoriasis—like how thick the plaques are and how much body surface area is involved,” says Bobby Buka, MD, a dermatologist at Bobby Buka MD Dermatology in New York City. It can also depend on what other medical conditions or medications the patient is on, the patient’s preferences and lifestyle, and the patient’s insurance coverage.
Typically, using a topical is the first line of treatment. But there are some caveats.
“If I’m treating a patient who also has psoriatic arthritis, then I wouldn’t just use topicals. I’d want to make sure we have some systemic agent on it. One of the scary things about psoriatic arthritis is that it’s irreversible, so I’d want to make sure we at least get in the way of some of that inflammation so we don’t have any permanent joint damage,” Dr. Buka adds.

What Causes Psoriasis, Exactly?
“Once a patient has more than 10% body surface area of psoriasis involvement, it gets difficult to just do topicals. It’s a lot of cream to rub on once or twice a day and the compliance really falls,” says Rhonda Q. Klein, MD, MPH, a dermatologist at Connecticut Dermatology Group.
The cost of treatments varies widely, and is typically based on your insurance and where you live. Using an app like GoodRx can help you figure out the cost of different medications in your area.
Topical medications
There are lots of different types of topical medications, like creams, solutions, and sprays that are applied directly to the skin. Some contain steroids, some contain a vitamin D analog, some contain a combination of steroids and a vitamin D analog, and some contain retinoids, for example. Topicals usually need to be applied once or twice a day.
The steroid creams tend to be more powerful, but can have more side effects, so Dr. Klein often advises patients to use a vitamin D topical during the week and a steroid topical on the weekend. This gives the skin a little break. “Whenever they’re having a psoriasis flare-up, I’ll have them use the steroid topical every day for two weeks,” she says.
Some topicals that were popular in the past, like cold tar products, are being phased out by many dermatologists because, although they work well, their smell turns off a lot of patients and they can stain clothes.
Oral medications
If topical treatments aren’t providing enough relief, a dermatologist may move on to a systemic treatment. There are pills that you can take anywhere from once weekly to twice daily. One that is commonly prescribed is called Apremilast.
Another option for some patients is acitretin, a vitamin-A derivative, but it can’t be used in women with childbearing potential because you can’t get pregnant within three years of taking it. There’s an increased risk of birth defects.
Other options like methotrexate and cyclosporine (which are chemotherapy drugs) may also be considered, though they can have serious side effects and require blood monitoring. “With methotrexate, you can have liver issues and cyclosporine can affect the kidneys and blood pressure,” says Dr. Klein.
Light or laser therapy
You can go to a dermatologist’s office two or three times a week to receive what’s called narrow-band UVB phototherapy. (Most dermatologists no longer use full-spectrum light that contains UVA rays because that would increase your risk for skin cancer.) It feels a lot like going to a tanning salon—you step into a vertical box that’s filled with lights.
“You don’t really see maximum benefit until 10 to 12 weeks and many patients continue to do it for six months,” says Dr. Klein. “There are also home light box units that we try to get insurance to cover.” Sometimes Dr. Klein will have patients use a combination of light therapy and a retinoid topical because the topical thins plaques and makes the skin more sensitive to light therapy.
There’s also an excimer laser, which is a form of ultraviolet laser and can be used in a doctor’s office two to three times a week. “It’s more of a targeted therapy and we actually put the laser in the areas where we see the plaques,” says Dr. Klein.
Biologics
“Biologic therapy is the hottest thing to hit dermatology and psoriasis in the last 10 years,” says Dr. Buka. It’s an injection or infusion that can be done weekly, every other week, every six weeks, or every three months, depending on the medication.
“Biologics are very safe and the success rate is in the 80 percent to 90 percent range,” says Dr. Buka. The downside is that they can be super expensive, so it’s a good idea to check with your insurance provider ahead of time to see what your out-of-pocket cost would be.
Though biologics are essentially a last-resort treatment, a lot of patients want to jump to them sooner these days because they’re very effective, not very time-consuming, and have few side effects. The issue is that some insurance companies require you to try cheaper drugs first before moving on to biologics.
So even though there is no cure for psoriasis, there are lots of treatment options that may help you find significant relief. “I think we’re getting better and better with our therapies and we’re getting longer remissions,” says Dr. Klein.
Source:-Prevention.com
Leave a Reply