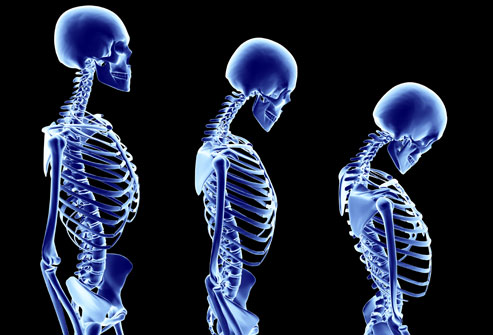
Osteoporosis is a very common bone disease that affects elderly people. It usually doesn’t present with any sign or symptom until you get injuries and fractures. For this reason, the condition is typically overlooked.
Postmenopausal osteoporosis is a medical condition that happens after menopause largely due to estrogen deficiency. It is characterized by having bones that are thinner, weaker, and more brittle.
According to the Centers for Disease Control and Prevention (CDC), the prevalence of osteoporosis of the lumbar spine in the United States is higher in women who are 65 years old and over (24.5%) than in men of the same age (5.1%).
In five to seven years following menopause, women can lose around 20% of their bone density. This is attributed to the drop in the level of estrogen after menopause, which helps maintain bone strength. Weaker bones can increase your risk of suffering from vertebral compression fractures, a fracture of the spine characterized by compression of the vertebra wherein the bone tissue collapses.
Risk Factors for Osteoporosis
Osteoporosis is a progressive disease with multiple causes. However, identified risk factors can increase your likelihood of having osteoporosis. The non-modifiable risk factors are age (over 65 years old), sex (women are more at risk, especially after menopause), and genetics (family history of osteoporosis).
Certain risk factors can be eliminated through lifestyle modification. These include:
Sedentary lifestyle. An inactive lifestyle can reduce muscle and bone mass, making you at risk of having fragile bones and osteoporosis.
Cigarette smoking and alcohol drinking. Smoking and alcohol drinking can result in lower bone density, which increases your risk of having fractures and osteoporosis.
Corticosteroids. Corticosteroids are medicines used to treat inflammation. Long-term use of corticosteroids is the most common cause of secondary osteoporosis.
Proton pump inhibitor. This drug is the most potent medication taken to reduce the production of stomach acid. Unfortunately, it also reduces the absorption of calcium in the stomach. Prolonged intake of proton pump inhibitors can put you at risk of having osteoporosis.
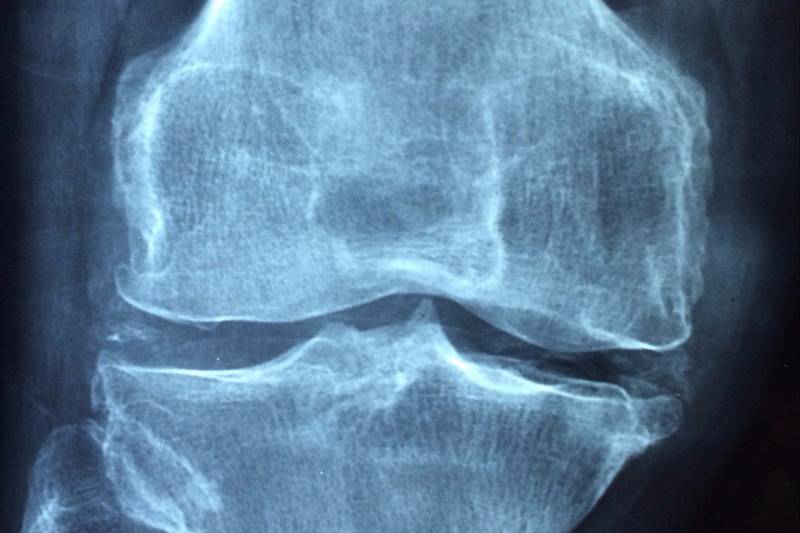
Living with Osteoporosis
Living with postmenopausal osteoporosis doesn’t have to be very restrictive. In fact, there are ways to make your life as normal as possible despite having to live with the disease.
1. Fall prevention
Women with postmenopausal osteoporosis have fragile bones, making them at risk of having fractures. For this reason, one of the most important concerns for patients with postmenopausal osteoporosis is safety. Remove tripping and slipping hazards at home like clutter, area rugs, and trailing wires. Consider using shower chairs, handheld showers, and non-slip bath mats in the bathroom. You can also install grab bars on your bathroom walls for additional support.
2. Healthy diet

Eating foods that are rich sources of calcium and protein can improve your bone density and reduce bone loss secondary to aging. Also, it has been shown that taking vitamin D supplements can decrease the rate of bone loss and incidence of fractures in older adults.
Moderate intake of alcoholic drinks is not harmful to your bones. However, long-term alcohol abuse is highly discouraged because it can harm and destroy your bone-forming cells.
3. Proper exercise
Leading an active lifestyle has been linked to having stronger bones. Women with postmenopausal osteoporosis find it harder to be physically active. You can set an appointment with your physical therapist to help you find an appropriate exercise for your condition. Doing therapeutic exercises have been shown to maintain and even increase the bone density of postmenopausal women and thereby reduce the risk of developing osteoporosis. Being physically fit can also give you stronger muscles that are essential for body coordination and structure.
4. Dealing with mobility
Postmenopausal osteoporosis can limit your mobility and affect your quality of life. You might find it difficult to twist or bend your body, rendering you incapable of attending to your personal needs. Using adaptive equipment like a dressing stick can help you put your clothes on without bending and twisting your body unnecessarily. You can also invest in mobility equipment like Pride Mobility Go Go Sport 3 Wheel Scooter to get to one point to another. To improve your mobility, you also need to strengthen your muscles by doing appropriate exercises.
5. Managing back pain
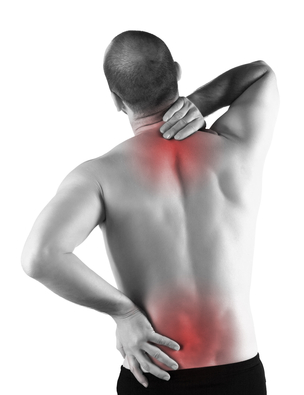
Back pain is one of the consequences of having postmenopausal osteoporosis. The most common reason for this is compression fractures of the vertebrae. Applying a heat pack or having warm showers can help ease tensed muscles and provide pain relief. If there is inflammation, applying a cold pack on the area can help reduce the swelling and pain. You can also wear back braces to support your back and relieve back pain.
Additionally, always be prepared by keeping a list of emergency numbers of the hospitals near your area. Equip yourself with a first aid kit so that you have an easy access to supplies in case of an emergency.
Leave a Reply